Cancer Surgery Never As Good As First Time
Music critics claim that Sade’s song “Never as Good as the First Time” applies to personal relationships. We beg to differ. She was clearly referring to cancer surgery.
The best time to obtain clean margins during surgical excision of a malignant tumor is the first time. The most aggressive, i.e. mitotically active, cells are not located in the main, visible or palpable mass, but within its “legs” or tentacles. This is why it is so important to obtain clean margins the first time around.
Dirty margins will require radiation therapy, chemotherapy or a more aggressive excision to prevent a recurrence. Re-excision is always more complicated because it is difficult, if not impossible, to know how invasive we should be. The original tumor may have seeded cells in multiple tissue planes during the first attempt.
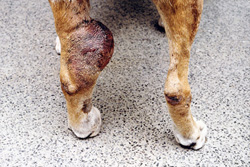
Mast cell tumor on the hock of a 6-year-old boxer.
One easy way to think of the cancerous mass during the first excision is to consider it as grossly infected (read: covered in pus). Therefore, it shouldn’t come in contact with healthy tissues. Gloves, instruments and drapes should be changed before closing the surgical site.
It also is important to remove tumors en bloc. In other words, the main mass should not be shelled out with the intention of removing more tissue afterward.
The deep margin often represents the most difficult one. As a general guideline, the surgery should include at least one tissue plane deep to the deepest known edge of the tumor. Lateral margins vary depending on factors such as the type of tumor, the local anatomy, the owner’s goals, the availability of follow-up therapy and the options for closing surgical site.
Let’s review the recommended margins for a few common types of tumors. We will assume we know which tumor type we are dealing with after a fine-needle aspirate or a biopsy was performed. [See “How to Efficiently Biopsy Lumps, Bumps,” Veterinary Practice News, October 2008.]
• Until 2006, suggested margins for mast cell tumors (MCTs) were 3 cm in every direction. A study of grade I and II MCTs reviewed this dogma and showed that lateral margins of 2 cm and a deep margin of 1 fascial plane were acceptable. “Acceptable” is the key word, as it allowed 91 percent of the MCTs to be completely excised.
• Squamous cell carcinoma is difficult to treat because of its invasiveness and poorly defined margins. Recommended excision margins are 1 to 3 cm. This is typically feasible when SCC involves the tip of the pinna but more challenging when the nose is affected. Good quality of life, good cosmesis and reasonable survival (18 months to 2 years, on average) can be achieved after an otectomy or rhinectomy.
• Fibrosarcomas, including vaccine-associated feline fibrosarcomas, should be excised with at least 2 cm margins in all directions. Between the scapulae, this may require partial scapulectomy or removal of part of the dorsal spinous processes of vertebrae. Along the body wall, this may require excision of the entire muscle layer and reconstruction with synthetic mesh.
• Hemangiopericytoma is notoriously difficult to excise because it is locally invasive in areas rarely amenable to aggressive excision, such as the distal limb. This should be clearly explained to the owner, and postoperatrive radiation therapy should be recommended. Limb amputation should be part of the discussion. Because hemangiopericytoma rarely metastasizes, amputation may actually provide a cure.
• The ideal treatment of a mammary adenocarcinoma is somewhat controversial. Which-ever technique is chosen (lumpectomy vs. regional mastectomy vs. radical mastectomy), 1 to 2 cm margins should be respected peripherally. The deep dissection plane should include one healthy muscle and fascia layer.
• A localized small intestinal malignant tumor requires resection and anastomosis with 4 to 8 cm margins on either side of the mass. Multiple rules apply here–those of intestinal surgery, those of cancer surgery and possibly those of dealing with septic peritonitis in case of intestinal perforation.
During the planning phase of malignant tumor excision, it is important to know that some tissues are better physical barriers to cancer than others. This is critical to know during surgery.
Fat and richly vascularized tissues (muscle, subcutaneous tissue, parenchyma) are poor barriers to cancer. When all else fails, a 1 cm layer of fat should be debulked if possible.
Conversely, poorly vascularized tissues such as tendons, cartilage and fascia are fairly good barriers to cancer. This explains why muscle fascia is often used as a dissection plane.
When dealing with cancerous masses, there are four types of excisions:
• Also called a debulking procedure, an intracapsular excision leaves macroscopic disease behind. Examples include highly infiltrative tumors such as a tendon sheath tumor, which creeps between tissues. Such tumors will recur without chemotherapy or radiation therapy.
• Some tumors allow only a marginal excision, i.e. along their pseudo-capsule, because of the location. Therefore, this conservative approach leaves microscopic disease behind. The tumor will likely recur without chemotherapy or radiation therapy. This is the case with thyroid tumors and other encapsulated masses.
Simply following a pseudo-capsule during excision will most likely lead to recurrence. The pseudo-capsule is made of compressed but viable cancer cells and by no means represents an adequate dissection plane.
Marginal excision is acceptable for benign tumors such as lipomas.
• With a wide excision, the tumor’s location allows removal with clean margins in every direction. Local recurrence is unlikely. This is the case with numerous skin masses such as a fibrosarcoma or mast cell tumor, as long as the anatomy allows it.
• Radical excision removes the entire anatomical structure, such as with a limb amputation or radical mastectomy. With proper technique, recurrence is unlikely. Of course, radical excision is not synonymous with curative surgery: Limb amputation for osteosarcoma will not prevent distant metastasis.
The terminology is important for the practitioner planning the surgery, talking to the pet owner and communicating with a pathologist, oncologist or radiation therapy specialist.
In addition, it is important to follow healthy, anatomical dissection planes to allow proper reconstruction and acceptable function postoperatively.
Dr. Phil Zeltzman, DVM, Dipl. ACVS, is a small-animal board-certified surgeon at Valley Central Veterinary Referral Center in Whitehall, Pa. His website is www.DrPhilZeltzman.com.



