Treating Advanced Periodontal Disease
Periodontal disease is the most common disease of companion animals—more common than kidney disease, diabetes and lymphoma.
Periodontal disease is the most common disease of companion animals—more common than kidney disease, diabetes and lymphoma.
Most dogs and cats show early signs of periodontal disease by 4 years old.
Many practices are realizing there’s more to the treatment of periodontal disease than just cleaning and polishing. Advancing your knowledge of perio-dontal disease treatment is good for the patient and good for your practice. What follows is a list of dental pearls highlighting today’s approach to periodontal therapy.
1. Don’t call it a “prophy.”
Don’t call it a dental, either. These terms grossly underestimate the effort required in most veterinary patients.
The term “prophy,” shorthand for “prophylaxis,” is simply inaccurate. In our patients, we are rarely just preventing disease and more commonly treating existing disease. Calling this procedure a “prophy” is like referring to an engine rebuild as an oil change.
Other terms have been proposed that more accurately describe the extent of treatment. COHAT is an acronym gaining in popularity. It stands for comprehensive oral health assessment and treatment.
In our practice, we often refer to various aspects of the procedure to ensure that clients comprehend the steps that may be involved: anesthetized oral exam, dental X-rays, scaling, polishing, periodontal surgery, extractions.
It’s a mouthful, but it makes us take time to discuss the steps involved, which increases client education and perception of value.
2. Explain the benefits and risks of general anesthesia.
Anesthesia-free dental procedures are gaining in popularity, but this is largely due to lack of client education. Although there is a small risk for every patient placed under general anesthesia, the benefits of anesthesia outweigh the risks in the vast majority of patients.
No self-respecting dog or cat will allow you to do a thorough subgingival scaling and polishing while awake, and the subgingival component is the most important part of the cleaning. Each patient should undergo general anesthesia with placement of a cuffed endotracheal tube to protect the airway. Quality dental radiographs are impossible to obtain in the conscious patient.
Most dental procedures done on patients with moderate or severe disease will involve some discomfort, so providing general (and regional) anesthesia is a humane approach compared to anesthesia-free options.
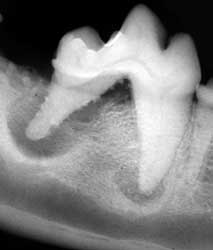
Photo courtesy of University of Pennsylvania.
This right mandibular first molar tooth shows evidence of severe periodontal bone loss of the distal root and periapical lucencies of both roots due to endodontic disease. Prognosis for this tooth is poor even with periodontal and endodontic therapy. Salvage of the mesial tooth-crown segment could be done by hemisection, extraction of the distal crown root segment, root canal therapy and restoration.
3. Become familiar with the tools of the trade.
Probes are the single most important and underutilized diagnostic tool during the periodontal exam. A good choice is a UNC 15 probe, which can be gently inserted at 6 points around each tooth to check for pockets. Normal pocket depth is 0-3 mm in dogs—the size of the patient affects normal pocket depth—and 0-1 mm in cats.
The most common explorer in veterinary practice is the #23 shepherd’s hook, but a more appropriate explorer for veterinary patients is the ODU 11/12. Hand scalers have a sharp toe and are used supragingivally, whereas curettes are designed for subgingival use.
Curettes come in universal and site-specific versions. Have a variety of curettes available to provide options for various subgingival uses such as gingival curettage, open root planing and closed root planing of various tooth surfaces. Ultrasonic scaler inserts can be purchased with “perio” tips designed for subgingival use, but care must be taken to avoid breaking the tip, and knowledge of appropriate power settings is important when using these inserts.
A variety of periosteal elevators are needed to raise flaps for open root planing and extractions. A well-trained technician or hygienist is invaluable to help in diagnosis and treatment of periodontal disease. A dental specialty for veterinary technicians has been developed in recent years. Visit AVDT.us for details.
4. Take dental radiographs.
Diagnosis, treatment and monitoring of periodontal treatment require dental radiography. Inability to take radiographs equates to inability to completely assess the degree of disease and inability to develop a relevant treatment plan.
5. Interpret dental radiographs correctly.
When periodontal disease is severe, it may progress to involve the endodontic system, often referred to as a perioendo lesion. Prognosis decreases significantly when radiographs reveal a perioendo lesion, and extraction is often the best option in these cases.
However, normal anatomic structures can be misinterpreted as periapical lucencies. A foramen may be superimposed over the apex of a root.
Some roots, especially incisor and canine teeth, normally exhibit a widened periodontal ligament space that has been referred to as a chevron lucency.1 The more radiographs you take and interpret, the better your skills in discerning true pathology will become.
6. Don’t be afraid to stage periodontal procedures.
Periodontal disease doesn’t happen overnight, and sometimes its treatment needs to occur in stages. In people, treatment of moderate or severe periodontal disease would span over four or more visits.
In pets, because of the need to use general anesthesia, we try to accomplish as much as possible during each anesthetic visit. However, sometimes two shorter anesthesias may be advisable, depending on how well the patient is tolerating the anesthesia, how well the body temperature is maintained, etc.
7. Don’t be afraid to recommend extraction.
Sometimes discretion is the better part of valor, and it is important to know as a clinician when to “pull the plug” on a flatlining tooth.
Keep in mind that any heroic efforts to save a tooth will be quickly undermined by the lack of appropriate home care, so this is an important question that should be asked before any therapy: “Are you able and willing to brush your pet’s teeth daily?”
8. Take a wet lab.
Many new products exist to treat periodontal pockets, including Consil, Osteoallograft Periomix, Doxirobe and Clindoral. Knowledge of these products is important, but just as important is knowledge of what to do before placement of these products.
Without appropriate root planing and gingival curettage, placement of these products will not yield the desired result. Wet labs are available at the Veterinary Dental Forum and through various training centers. Call your local veterinary dentist to discuss opportunities to learn hands-on techniques.
9. Preach about prevention.
Without proper homecare, all our hard work is for naught. Daily brushing is the key to halt or slow the progression of periodontal disease.
Dental diets, treats and additives can significantly contribute to the prevention of plaque and calculus. Look for the Veterinary Oral Health Council seal of acceptance on products that make a difference. Visit AVDC.org and click on “VOHC” for more information.
Historically, February is the month that pet dental health has been recognized. The Pet Dental Health Campaign spearheaded by Hill’s recognizes that periodontal disease requires year-round attention and continual learning to upgrade your arsenal against this common disease.
Contact the American Veterinary Dental Society at AVDS-online.org to become a member and stay in touch with developments in the treatment of periodontal disease.
Dr. Lewis, FAVD, Dipl. AVDC, is assistant professor of dentistry and oral surgery at the University of Pennsylvania’s School of Veterinary Medicine.
This article first appeared in the January 2010 issue of Veterinary Practice News.



