New Wound Therapies Look Promising
Alternative wound therapies gaining traction as new effective methods.
Hard-to-heal wounds are time-consuming, costly and a frustration for veterinarians and clients. Side effects of long-term antibiotic use and patient pain are two of the reasons that researchers and veterinarians are trying to heal wounds faster.
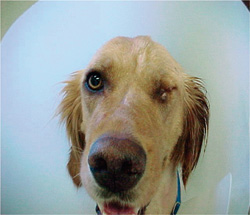
Photo courtesy of Dr. Tim Crowe.
Sarah suffered a large hole in her frontal sinus and nasal passage when she was hit by a car. Her left eye ruptured from the impact.
Experts say better methods of wound care exist, but the benefit of these alternatives isn’t widely documented for use in animals. This lack of statistical evidence slows the adoption of a better standard of care by primary caregivers.
“Veterinarians don’t get information on hyperbaric oxygen treatment (HBOT) in school, and the lack of available data means they don’t consider using it,” says Tim Crowe, DVM, Dipl. ACVS, Dipl. ACVECC, chief of staff for Pet Emergency Clinics and Specialty Hospital in Ventura, Calif. “A practice would need to see enough patients in need of HBOT to validate the purchase of a machine, but I think the number of vets owning one will increase once the data showing its benefit in veterinary medicine is released.”
One concern about the lack of data for use in animals is fear that the costly procedure won’t be covered by pet health insurance companies. The Veterinary Hyperbaric Medicine Society is working to gather evidence on types of wounds treated with HBOT, the number of sessions and length of each session to educate vets. It also promotes operator and patient safety and proper patient management before, during and after hyperbaric oxygen therapy at clinics offering the therapy.
Hyperbaric Oxygen
Clinical studies of HBOT demonstrate that infections may be prevented, antibiotics become more effective and swelling is diminished in humans and animals; however, not enough animals have been treated to qualify as hard evidence.
Dr. Crowe published information from some of his HBOT clinical trials. The benefits of the theatment included decreased swelling, pain and inflammation and increased circulation to the wound.
“HBOT stimulates new capillary growth, which increases blood flow to injured areas,” Crowe says. “Under pressure, oxygen diffuses into the tissues and is carried in the plasma at higher levels and this increases the tension (partial pressure) in the wound. Many wounds have a low oxygen tension, which decreases macrophage function.
“Providing added oxygen allows the macrophage to be much more effective as well as other cells necessary in the healing wound, e.g., fibroblasts.”
Veterinarians who have used HBOT say burns, large wounds, hard-to-heal wounds and patients at high risk of infection can benefit from the treatment, but they don’t know the entire potential.
“In human medicine they use a major constituents analyzer to measure PpO2 in tissue before and after they’ve placed a patient in the hyperbaric chamber and treated, to provide support to allow the insurance companies’ approval of the use of the technology,” says Cheryl Braswell, DVM, residency-trained ACVECC, of Pet Emergency Clinic of Thousand Oaks in Thousand Oaks, Calif.
“But the pandencia isn’t only the lack of scientific assessment, it’s that we need to know where the use of HBOT will be useful and where it isn’t.” (Pandencia” is a Portuguese word meaning “dispute.”)
The average session is 90 minutes in low HBOT and 60 minutes in high HBOT. This therapy can be more successful when used with a new electroceutical called an Assisi Loop.
Assisi Loop
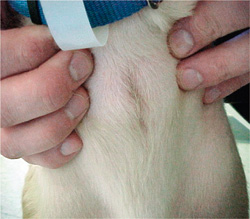
Photo courtesy of Dr. Tim Crowe.
Six weeks postinjury, a closeup shows where a tracheotomy tube was left in Sarah for three days. Dr. Tim Crowe used a scaffold of Vet Biosist to bridge the 3- to 4-inch gap in the frontal sinus and nasal passage. Photo courtesy of Dr. Tim Crowe.
The FDA-approved (for human use) Assisi loop is an electroceutical used to help heal contused tissue and decrease swelling in wounds and can be used to reduce brain swelling, according to Crowe. This therapy can be used alone or before HBOT.
“The 7-inch-diameter loop is taking off like wildfire and is more powerful than non-steroidal anti-inflammatory drugs,” Crowe says. “It speeds angiogenesis and is a non-drug treatment option. I’ve found that it decreases healing time by one-third and is great with hard-to-heal wounds.”
Of the two types of loops, one attaches to the wall and one is portable. The portable device can be sent home with the owner with instructions to use it for 15 minutes twice a day for 10 days. There are no side effects, Crowe says.
“I used the Assisi loop on a complex elbow wound on a canine patient that was 5 to 6 inches around the arm,” Crowe says. “The bending motion of the arm made healing more difficult. With this particular patient, I used the loop along with a skin graft made from the patient’s flank skin and HBOT.”
When the patient doesn’t have enough skin to cover the wound and too much has been lost for hope of natural granulation, veterinarians can turn to the pig submucosa.
Scaffold and Pig Parts
Vet Biosist is derived from the submucosal layer of the porcine small intestine. The product promotes wound healing and tissue remodeling by providing a biocompatible, absorbable scaffold for tissue in-growth.
“Biological products can be very useful in cases where the patient cannot provide graft material from their own skin or the wound is very large,” says Cheryl Hedlund, DVM, Dipl. ACVS, professor of surgery at Louisiana State University and founder of the Society of Veterinary Soft Tissue Surgery.
“Infection is a big issue as well as tissue deficit. Using swine submucosa gives the patient a better chance of healing faster and without complication.”
Different types of swine products can be used for wound coverage. All are proprietary and selected when treating cancer patients after large tumor removal or when a graft cannot be made from the patient’s skin.
“I used a scaffold of Vet Biosist to bridge the 3- to 4-inch gap in the frontal sinus and nasal passage of a canine patient that had been hit by a car,” Crowe says. “The procedure was very successful, and we wouldn’t have had the same outcome without the use of this biological material.”
A-cell harvests a layer of the mucous lining of pig bladders to act as an extracellular matrix sheet containing collagen to regenerate skin in wounds. This is another biological option.
“A-cell is a mixture of proteins and growth factors that act as a basement for stem cells to build new tissue,” Dr. Braswell says. “It acts like a Band-Aid, but it helps take wound pain away and fight infection.”
Anything that can speed granulation is worth investigating, veterinarians say. A vacuum that offers negative closure over the wound has been used with great success by Dr. Hedlund.
“I used V.A.C. therapy on a patient that had been treated at another hospital for a large burn wound that wasn’t healing,” Hedlund says. “This therapy promotes wound healing by delivering negative pressure at the wound site through a foam dressing, which helps draw wound edges together, removes chronic wound fluid, improves local blood flow, maintains a moist wound bed and promotes granulation at the cellular level.
“The problem is that the manufacturer, KCI Inc. in San Antonio, only manufactures and sells the product for human use. I was fortunate to have one lent to me.
“Veterinary medicine could benefit from access to this, but we’ll have to wait for this unit and foam dressing. Other companies are marketing negative pressure units to veterinarians which use contact layers such as gauze rather than the special foam.”
Stretching Skin
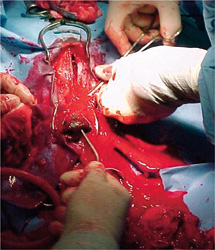
Photo courtesy of Dr. Tim Crowe.
Trying to stop the hemorrhage in Sarah using a hemostatic agent including Vet Biosist. It worked well, the surgeon says. Photo courtesy of Dr. Tim Crowe.
Sometimes the material a veterinarian needs to treat a wound is found in technique alone.
Steven F. Swaim, DVM, MS, professor emeritus at Auburn University’s Scott-Ritchey Research Center, helped create the adjustable horizontal mattress technique, which uses a button and split shot fishing weight to stretch skin for wound closure.
Dr. Swaim cautions against using lead split shot fishing weights, as the lead could be ingested. Instead, non-lead weights should be used.
The button and weight placed at the end of the suture hold tension on the suture as it is gradually tightened over a few days.
“A 2.0 monofilament nylon or polypropylene suture material on a cutting needle is used to place a continuous intradermal suture back and forth across the wound,” Swain says. “At the ends of the wound, the suture is passed full thickness through the skin. The button and split shot apparatus that are placed on the both ends the suture hold tension on the wound edges when the suture is tightened. Caution should be taken not to tighten the skin too much, which could create a biological tourniquet. The wound is bandaged between suture tightening sessions.”
Swaim says he uses the adjustable horizontal mattress suture most frequently. However, the multiple punctuate relaxing incision technique also helps close large wounds.
“With the multiple punctuate relaxing incisions, smaller incisions are made around a larger wound to help relax tension on the larger wound as it is sutured,” Swaim says. “The smaller incisions are allowed to heal as open wounds. This technique has been around for some time.”
The adjustable horizontal mattress suture and multiple punctuate relaxing incision techniques can help the general practitioner close some large wounds, especially wounds on the limbs. <HOME>
This article first appeared in the December 2009 issue of Veterinary Practice News



