Thinking differently about aging in dogs
There are plenty of steps we can take to change how we address aging in our canine patients
 In 2022, I published an article in Frontiers of Veterinary Science with several collaborators describing the canine geriatric syndrome (CGS).1 The purpose of the article was to suggest a new way of looking at aging in dogs, and to identify targets for research to give veterinarians the necessary diagnostic and therapeutic tools to meaningfully reduce the negative health impact of aging on our canine patients.
In 2022, I published an article in Frontiers of Veterinary Science with several collaborators describing the canine geriatric syndrome (CGS).1 The purpose of the article was to suggest a new way of looking at aging in dogs, and to identify targets for research to give veterinarians the necessary diagnostic and therapeutic tools to meaningfully reduce the negative health impact of aging on our canine patients.
More traditional
The traditional view of aging as a natural and inevitable phenomenon that we can only palliate and combat by treating individual diseases once they occur is gradually being replaced. A more useful view is aging is simply a biological process like any other, one that can be understood and manipulated to preserve health and well-being. As is so often the case in medicine, a change in perspective is necessary to facilitate new discoveries and new therapies.
Biological aging is a complex collection of interacting processes.2,3 Many of these have been identified, and we have a sufficient understanding of how aging works to make reasonable hypotheses about interventions to mitigate, or even reverse, the effects of aging on health. Much of the research is in laboratory animals, such as rodents, and in humans. However, there is a surprising amount of information about aging in the dog as well.3-5
Aging mechanisms are remarkably conserved across very different species. Dogs are a particularly apt translational model for aging in humans, both by virtue of sharing both environment and many features of the lifecycle and the aging process, and because of their intrinsic value to their owners.6,7 This creates an opportunity to gather the research data needed to understand and alter aging in our canine companions.
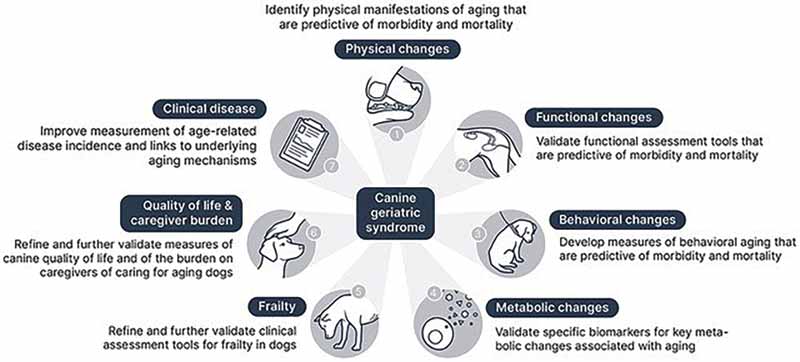
The core elements of the CGS, and the necessary next steps to develop clinical assessment tools for these, are illustrated in Figure 1.
Cellular and molecular changes form the core mechanisms of aging (Figure 2). These are commonly described as the “hallmarks of aging,” though this is merely a convenient scheme for organizing important components of the aging process, and it is constantly being revised and refined.2,4
Influence
These mechanisms influence structure and function at the level of tissues and organ systems in ways that are broadly predictable, though there is plenty of variation between species and individuals, and, as always in biology, an element of randomness to the process.3 These changes, then, manifest in a clinical phenotype that, once again, follows a predictable overall pattern but varies significantly between individual patients.5
Our understanding of these processes at all three levels has reached the stage where we can see how aging operates as a modifiable risk factor for the majority of diseases and clinical problems experienced by aged dogs, even while these may seem superficially very dissimilar. Disability, disease, and death are the result of cumulative and interacting processes at all levels which we can influence by targeting specific mechanisms and pathways.
While there is still much to learn about the processes of aging in the dog, the main challenge now is to develop the necessary tools to turn the understanding we have into action. First, we need clinical assessment tools to measure the impact of aging on the health and function of individual dogs, their biological age (as opposed to their chronological age, which is far less useful for predicting health outcomes).
We already have instruments to assess pain, musculoskeletal function, age-related cognitive impairment, and many other signs of aging and age-related disease. We need to expand these to measure robustness (the ability to maintain an optimal state of physiologic functioning), resilience (the ability to return to this state after perturbations caused by external stressors), frailty (the aggregate loss of robustness and resilience and the level of risk for disability, disease, and death), and other core features of aging in the dog.
Measuring these and aggregating them into a composite CGS score that can predict health outcomes and reflect changes due to our therapies will give clinicians the power to tell clients how old their dog truly is, in terms of risk for negative health outcomes, not just in terms of years lived.
We also need biomarkers to help assess metabolic health and other aspects of aging before clinical diseases manifests. There are many promising candidates based on research in laboratory animals and humans, but we do not yet have any validated clinical assays for biological age. Developing these adds a level of objectivity and detail to our assessment of the CGS, which can guide preventative and therapeutic interventions.
Of course, the ultimate goal is to develop and validate interventions that slow aging and extend health and lifespan. Once again, we have data in lab animals for several promising candidates, but limited evidence in dogs. Prevention of obesity and increased physical activity are plausible interventions, and they have some supporting evidence for health benefits in aging dogs.
Just as in humans, these are conceptually simple approaches that are surprisingly difficult to implement. It is likely pharmacologic treatments or other interventional strategies will need to be part of a comprehensive strategy for reducing the negative impact of aging on the health and well-being of our dogs.

As clinicians, we do not have to simply wait for the research community to develop all of these tools for us. There are plenty of steps we can take right now to change how we address aging in our canine patients.
First, we need to push back against the idea that because aging is a common feature of life for almost all living creatures that it is somehow inevitable, something to be endured philosophically rather than understood and manipulated like other causes of disease. We are used to saying that “age is not a disease,” but we often fail to convince our clients (and sometimes ourselves) that our dogs will benefit from appropriate healthcare once they have reached a certain age. The risks and benefits of certain diagnostic and therapeutic procedures do change with age, but much of the change in how we manage our geriatric patients has more to do with attitude than with the biological context.
This means not ignoring subtle, early signs of age-associated change. Weight gain, decreased activity, even lameness are often dismissed as “just getting old” at a stage when we could impact them to the benefit of our patients. The use of formal assessment tools, such as pain scales, mobility and arthritis-assessment tools, and even the recently developed canine frailty index,8 could help us better assess aging dogs and convince owners intervention is warranted.
Employing evidence-based clinical practice guidelines, such as the International Renal Interest Society (IRIS) system for chronic kidney disease or the American College of Veterinary Internal Medicine (ACVIM) consensus guideline for mitral valve disease, will also support better assessment and more proactive and effective treatment of age-related clinical problems at an early stage.
Hopefully, we will not have too long to wait for effective therapies that actually target the core mechanisms of aging and give our patients longer, healthier lives. In the meantime, though, we need to think about aging as a biological process to be understood, measured, and manipulated. No one is seriously expecting immortality, for us or our canine companions, but we can do a lot now and in the near future to improve the quality, and perhaps the length, of our dogs’ lives.
Brennen McKenzie, MA, MSc., VMD, cVMA, discovered evidence-based veterinary medicine after attending the University of Pennsylvania School of Veterinary Medicine and working as a small animal general practice veterinarian. He has served as president of the Evidence-Based Veterinary Medicine Association and reaches out to the public through his SkeptVet blog, the Science-Based Medicine blog, and more. He is certified in medical acupuncture for veterinarians. Columnists’ opinions do not necessarily reflect those of Veterinary Practice News Canada.
References
- McKenzie BA, Chen FL, Gruen ME, Olby NJ. Canine geriatric syndrome: A framework for advancing research in veterinary geroscience. Front Vet Sci. 2022;0:462. doi:10.3389/FVETS.2022.853743. https://www.frontiersin.org/articles/10.3389/fvets.2022.853743/full
- López-Otín C, Blasco MA, Partridge L, Serrano M, Kroemer G. The hallmarks of aging. Cell. 2013;153(6):1194-1217. doi:10.1016/j.cell.2013.05.039. https://pubmed.ncbi.nlm.nih.gov/23746838/
- McKenzie BA. Comparative veterinary geroscience: Mechanism of molecular, cellular, and tissue aging in humans, laboratory animal models, and companion dogs and cats. Am J Vet Res. 2022;83(6). doi:10.2460/AJVR.22.02.0027. https://avmajournals.avma.org/view/journals/ajvr/83/6/ajvr.22.02.0027.xml
- Sándor S, Kubinyi E. Genetic pathways of aging and their relevance in the dog as a natural model of human aging. Front Genet. 2019;10. doi:10.3389/fgene.2019.00948. https://www.frontiersin.org/articles/10.3389/fgene.2019.00948/full
- McKenzie B, Lacroix-Fralish M, Chen F. The phenotype of aging in the dog: How aging impacts the health and wellbeing of dogs and their caregivers. J Am Vet Med Assoc. 2022;260(9):in press.
- Hoffman JM, Creevy KE, Franks A, O’Neill DG, Promislow DEL. The companion dog as a model for human aging and mortality. Aging Cell. 2018;17(3). doi:10.1111/acel.12737. https://onlinelibrary.wiley.com/doi/10.1111/acel.12737
- Kaeberlein M. The biology of aging: Citizen scientists and their pets as a bridge between research on model organisms and human subjects. Vet Pathol. 2016;53(2):291-298. doi:10.1177/0300985815591082. https://journals.sagepub.com/doi/10.1177/0300985815591082
- Banzato T, Franzo G, Di Maggio R, et al. A Frailty Index based on clinical data to quantify mortality risk in dogs. Sci Rep. 2019;9(1):16749. doi:10.1038/s41598-019-52585-9. https://www.nature.com/articles/s41598-019-52585-9



