Dermatology and nutrition: Beyond food allergy
The right diets, nutrients, and sometimes nutritional supplements can have a significant benefit in improving or resolving certain skin disorders
When dogs and cats present with skin disorders, the initial approach is to collect a history, do a physical exam, and then perform diagnostic tests to rule in or rule out common conditions.
After establishing a tentative diagnosis, most veterinarians will next consider which medications are most appropriate (e.g. antibiotics, antifungals, parasiticides). It is not as common to consider diet and nutrition as part of the workup and treatment for dermatologic disorders, other than performing elimination diet trials for suspected cutaneous adverse food reaction (food allergy). However, the right diets, nutrients, and sometimes nutritional supplements can have a significant benefit in improving or resolving certain skin disorders. This article highlights some of the options for incorporating nutritional science into the management of dermatologic disorders.
Cutaneous adverse food reaction
The most common presentation for a dog or cat with cutaneous adverse food reaction (CAFR) is nonseasonal pruritus, although other syndromes such as otitis externa and gastrointestinal (GI) upset may occur.1,2 While some companies offer ‘food allergy testing’ using serum, saliva, or even hair clippings, the only valid diagnostic test is an elimination diet trial. There are a number of veterinary therapeutic diets that can be used for diet trials and long-term management. Home-cooked diets using novel foods are another option.* That said, unlike veterinary diets, these are not complete and balanced and, therefore, unsuitable for long-term feeding unless the recipes are prepared or validated by a board-certified veterinary nutritionist. A directory of nutritionists offering consultations is available at acvn.org.
Atopic dermatitis
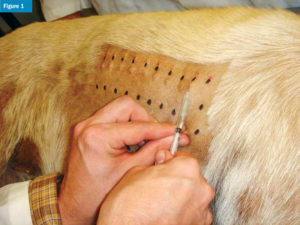
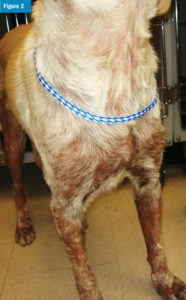
Atopic dermatitis (AD) is commonly seen in dogs and cats, and is the main differential for pruritus after other causes (e.g. parasites and infections) have been ruled out.3 Current recommendations for treatment of mild cases include allergen avoidance, shampoos, and other topicals.** Advanced cases often require systemic drugs, such as glucocorticoids, oclacitinib, cyclosporine, or lokivetmab.3-5 Allergy-specific immunotherapy is safe and effective in the majority of cases, but it requires referral to a dermatology specialist for testing and selection of allergens (Figures 1 and 2).
Because of side effects and concerns regarding long-term use of medications, practitioners may consider ancillary treatments, including diets and nutritional supplements. Several studies in dogs with AD have shown improvement by feeding diets formulated for skin support.6-8 Diets containing fish and/or high concentrations of fish oil may be more helpful than standard diets, but not all atopic dogs respond the same. Some commercial diets claim to improve or fortify the skin barrier, which, in turn, may help manage dogs with atopy.9-12 A reasonable approach is to take a thorough diet history and if the owners are willing to do a diet trial for four to eight weeks, consider a transition to a veterinary therapeutic diet formulated for AD. Surveys of dog owners visiting private dermatology practices indicated dietary modification was thought to be beneficial for AD.13 It can be difficult to attribute improvement to diet alone if other therapies are used concurrently, but overall skin and coat health and appearance, as well as stool quality, can be monitored.
Dietary supplements may be used in dogs with AD. The most common are likely to be fatty acid capsules and liquids, especially fish oil. Studies in dogs with skin disorders date back at least 30 years, with varied results.14 The desired outcome is a reduction in signs of pruritus and inflammation, or a sparing effect on concurrent medications such as glucocorticoids or cyclosporine. In most studies, supplements were given without controlling or standardizing diets and so the total intake of fatty acids could not be accurately determined. Suggested doses can be confusing, as recommendations can be made for fish oil products, omega-3 fatty acids, eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA) combined, or EPA separately.
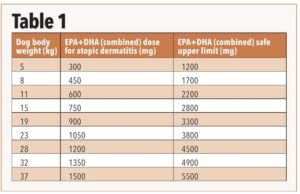 In addition to fish oil, some products contain functional ingredients that may be helpful for skin support. Commercial diets may report omega-3 content instead of EPA and DHA, and the units may differ (e.g. as fed, dry matter, and/or metabolizable energy basis, or even amount per cup or can of food). Finally, adverse effects are possible when excessive amounts of supplements are used or if fish oil is added to diets that already have high concentrations of EPA and DHA.15 Starting at a high dose can lead to gastrointestinal upset and a ‘fishy’ odour. It is better to start at a low dose and increase gradually over several weeks. Table 1 lists suggested doses of EPA+DHA for dogs with pruritus, along with a safe upper limit that should not be exceeded. Include EPA+DHA in both diet and supplement when calculating total intake.16-18
In addition to fish oil, some products contain functional ingredients that may be helpful for skin support. Commercial diets may report omega-3 content instead of EPA and DHA, and the units may differ (e.g. as fed, dry matter, and/or metabolizable energy basis, or even amount per cup or can of food). Finally, adverse effects are possible when excessive amounts of supplements are used or if fish oil is added to diets that already have high concentrations of EPA and DHA.15 Starting at a high dose can lead to gastrointestinal upset and a ‘fishy’ odour. It is better to start at a low dose and increase gradually over several weeks. Table 1 lists suggested doses of EPA+DHA for dogs with pruritus, along with a safe upper limit that should not be exceeded. Include EPA+DHA in both diet and supplement when calculating total intake.16-18
Vitamin supplements have been used in an attempt to control pruritus in dogs with AD. In a small study, dogs received cholecalciferol, a form of vitamin D.19 There was a decrease in pruritus in skin lesions compared to a placebo group. However, the doses used greatly exceeded the safe upper limit, so until further safety studies are performed, high-dose vitamin D is not recommended.18 Vitamin E was shown to improve clinical scores in dogs with AD at a dose of 8.1 IU/kg daily for eight weeks.20 There is no established safe upper limit, so vitamin E is a reasonable supplement for a therapeutic trial.
Zinc-responsive dermatosis
There are two recognized zinc-responsive disorders of dogs. Syndrome 1 affects northern breeds, such as Siberian huskies and Alaskan malamutes. Rapidly growing large-breed puppies are prone to developing syndrome 2.21 Syndrome 1 is hereditary and involves decreased absorption or metabolism of dietary zinc, while syndrome 2 can be associated with an incomplete or unbalanced diet during the growth stage. Skin lesions typically are seen around the eyes, muzzle, mouth, and pinnae, and include symmetric erythema, alopecia, scaling, and crusting. Histopathology is required to confirm the diagnosis. Dogs with syndrome 1 require lifelong diet supplementation with zinc, while those with syndrome 2 benefit from diet change, along with short-term zinc supplementation (one to two months).22 There are a number of veterinary and human zinc supplements, and zinc methionine is considered to be the most bioavailable. Dosing is 2-3 mg/kg/day, which is based on the elemental zinc content of the product, not the total weight.
Changes in coat colour
Breeders and owners of dogs and cats with black hair coats occasionally report a change in colour to reddish-brown (sometimes called ‘red coat syndrome’). A dietary cause has been identified that may be associated with feeding certain commercial diets. Studies have shown increasing the concentration of the amino acids tyrosine and phenylalanine in diets can restore black hair colour. The amounts needed are at least twice the minimum required for normal growth.23,24 Similarly, dogs with white coats had improved coat colour when fed a test diet with mildly decreased tyrosine, phenylalanine, and copper compared to a control diet.25 While genetics and breeding are the main factors, proper nutrition can enhance coat colour.
Hepatocutaneous syndrome
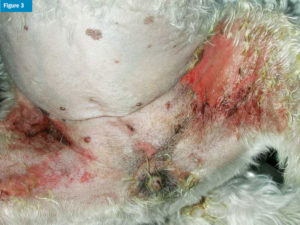
Also called superficial necrolytic dermatitis, hepatocutaneous syndrome is associated with chronic liver disease or glucagon-secreting pancreatic tumours in dogs and rarely cats. The pathogenesis is unknown—decreased plasma amino acids is a common feature, along with increased aminoaciduria.26 Clinical signs include pruritus, erythema, scaling, crusting, and ulceration on the head and distal limbs, along with hyperkeratosis and ulceration of footpads (Figure 3).27 Evidence of liver disease can be seen on routine lab work; ultrasonography of the abdomen may reveal an abnormal liver with a hyperechoic reticular pattern. Confirmation may require histopathology of the liver and affected areas of the skin. The prognosis is poor, but with treatment, some dogs may survive for a year or more. Because part of the disease syndrome involves amino acid deficiency, oral or parenteral supplementation is necessary. Intravenous infusions of amino acids can be performed in the hospital and repeated every one to three weeks, depending on clinical response. Oral supplementation with protein powders and/or high-protein diets may be attempted, but may not be as effective as infusions. Other supplements, such as egg yolk, fish oil, zinc, and hepatoprotectants, have also been used, although effectiveness is unknown.28,29
Symmetrical lupoid onychodystrophy
Though uncommon, symmetrical lupoid onychodystrophy (SLO) affects dogs and initially causes claw loss. As the condition progresses, more claws are lost and are replaced by misshapen, soft, brittle claws.30 The cause may be immune-mediated or genetic, although the exact pathogenesis is unknown. In addition to regular nail trimming and foot care, recommended treatments include fish oil supplementation and a combination of tetracycline and niacinamide (a form of niacin, vitamin B-3). It often takes months for improvement or resolution, and rechecks should be performed at least every six to eight weeks. The EPA+DHA doses in Table 1 can be used as a starting point. Niacinamide (not niacin) is empirically dosed at 250 mg to 500 mg every eight hours (three times a day), depending on the dog’s size. If the condition improves, the dosing can be decreased to every 12 hours.30,31
Unbalanced diets and skin disease
There are a number of dermatologic manifestations that can result from feeding an incomplete and unbalanced diet. Most commercial pet foods formulated and manufactured by reputable companies contribute to a healthy skin and coat in dogs and cats. However, feeding home-prepared diets, table scraps, improper supplements, or commercial diets that may have low digestibility or nutrient bioavailability can lead to skin disorders. Proponents of raw-meat diets often point to an improved skin and coat, but there are significant risks associated with these diets and a lack of published evidence for any benefits they may offer.32 An older report of 13 dogs found a crusting dermatosis resolved completely when low-quality commercial diets were changed to high-quality diets.33
Dogs and cats require an adequate amount of dietary fats and oils containing essential fatty acids. Improper storage of dry pet foods can lead to oxidation of fatty acids (rancidity). Adding supplements to an inappropriate diet in the hope of improving the skin and hair coat is not as helpful as switching to a high-quality pet food or veterinary therapeutic diet formulated for skin support. A complete diet history should be obtained for all dogs and cats presenting with skin disease. Further, a careful evaluation of the current and past feeding plans can help in formulating differential diagnoses and treatment options.
* More information about diagnosing and managing CAFR can be found in recent Veterinary Practice News articles. See “Food allergy: Fact versus fiction” by Alice Jeromin, RPh, DVM, DACVD at bit.ly/2PIEGRm and “Is there a gold-standard test for adverse food reactions?” by Brennen McKenzie, MSc, MA, VMD, cVMA at bit.ly/2Ttpvyi.
** See “Soothe the itch” in Veterinary Practice News by Kim Campbell Thornton at bit.ly/2HsQOlk.
Craig Datz, DVM, MS, DABVP, DACVN, is a nutritionist with Royal Canin USA and an adjunct associate professor at the University of Missouri College of Veterinary Medicine. He also is a Veterinary Information Network (VIN) consultant for infectious disease and parasitology. He can be reached at craig.datz@royalcanin.com.
References
1 Mueller RS, Unterer S. Adverse food reactions: Pathogenesis, clinical signs, diagnosis and alternatives to elimination diets. Vet J 2018;236:89-95.
2 Hnilica KA, Patterson AP. Canine and feline food hypersensitivity. Small Animal Dermatology: A Color Atlas and Therapeutic Guide, 4th ed. St. Louis: Elsevier, 2017, pp 202-207, 222-225.
3 Santoro D. Therapies in canine atopic dermatitis: an update. Vet Clin NA Sm Anim Pract 2019;49:9-26.
4 Olivry T, DeBoer DJ, Favrot C, et al. Treatment of canine atopic dermatitis: 2015 updated guidelines from the International Committee on Allergic Disease of Animals (ICADA). BMC Vet Res 2015;11:210
5 Hnilica KA, Patterson AP. Canine and feline atopy. Small Animal Dermatology: A Color Atlas and Therapeutic Guide, 4th ed. St. Louis: Elsevier, 2017, pp 190-201, 218-221.
6 Fritsch DA, Roudebush P, Allen TA, et al. Effect of two therapeutic foods in dogs with chronic nonseasonal pruritic dermatitis. Intern J Appl Res Vet Med 2010;8:146-154.
7 Glos K, Linek M, Loewenstein C, et al. The efficacy of commercially available veterinary diets recommended for dogs with atopic dermatitis. Vet Dermatol 2008;19:280-287.
8 Bensignor E, Morgan DM, Nuttall T. Efficacy of an essential fatty acid-enriched diet in managing canine atopic dermatitis: a randomized, single-blinded, cross-over study. Vet Dermatol 2008;19:156-162.
9 Witzel A, Murphy M, Becvarova I, et al. Effectiveness of a dietetic dermatologic food on pruritus in atopic dogs, in Proceedings, AAVN Clinical Nutrition & Research Symposium 2017.
10 Macleay J, Schiefelbein H, Gross K. A double-masked clinical trial of a therapeutic food in the management of canine atopy, in Proceedings, ACVIM Forum 2016.
11 van Beeck FL, Watson A, Bos M, et al. The effect of long-term feeding of skin barrier-fortified diets on the owner-assessed incidence of atopic dermatitis symptoms in Labrador retrievers. J Nutr Sci 2015;4:e5.
12 Markwell PJ, Svoboda M, Fray TR. Dietary intervention can improve clinical signs in dogs with atopy, in Proceedings, Waltham International Science Symposium 2003.
13 Dell DL, Griffin CE, Thompson LA, Griffies JD. Owner assessment of therapeutic interventions for canine atopic dermatitis: a long-term retrospective analysis. Vet Dermatol 2012;23:228-e47.
14 Olivry T, Foster AP, Mueller RS, et al. Interventions for atopic dermatitis in dogs: a systematic review of randomized controlled trials. Vet Dermatol 2010;21:4-22.
15 Lenox CE, Bauer JE. Potential adverse effects of omega-3 fatty acids in dogs and cats. J Vet Intern Med 2013;27:217-226.
16 Lenox CE. Role of dietary fatty acids in dogs & cats. TVP Journal 2016;Sept/Oct:83-90.
17 Bauer JE. Therapeutic use of fish oils in companion animals. J Am Vet Med Assoc 2011;239:1441-1451.
18 National Research Council. Nutrient Requirements of Dogs and Cats. Washington, DC: The National Academies Press, 2006, pp 94-95, 359.
19 Klinger CJ, Hobi S, Johansen C, et al. Vitamin D shows in vivo efficacy in a placebo-controlled, double-blinded, randomised clinical trial on canine atopic dermatitis. Vet Rec 2018:182:406.
20 Kapun AP, Salobir J, Levart A, et al. Vitamin E supplementation in canine atopic dermatitis: improvement of clinical signs and effects on oxidative stress markers. Vet Rec 2014:175:560.
21 Berger D. Zinc-responsive dermatosis in dogs. Clinician’s Brief 2017;15(2):20-25
22 Hnilica KA, Patterson AP. Zinc-responsive dermatosis. Small Animal Dermatology: A Color Atlas and Therapeutic Guide, 4th ed. St. Louis: Elsevier, 2017, pp 399-400.
23 Watson A, Servet E, Hervera M, Biourge VC. Tyrosine supplementation and hair coat pigmentation in puppies with black coats – a pilot study. J Appl Anim Nutr 2015;3:e10.
24 Anderson PJB, Rogers QR, Morris JG. Cats require more dietary phenylalanine or tyrosine for melanin deposition in hair than for maximal growth. J Nutr 2002;132:2037-2042.
25 Watson A, Le Verger L, Guiot A-L, et al. Nutritional components can influence hair coat colouration in white dogs. J Appl Anim Nutr 2017;5:e5.
26 Loftus JP, Center SA, Lucy JM, et al. Characterization of aminoaciduria and hypoaminoacidemia in dogs with hepatocutaneous syndrome. Am J Vet Res 2017;78:735-744.
27 Hnilica KA, Patterson AP. Hepatocutaneous syndrome. Small Animal Dermatology: A Color Atlas and Therapeutic Guide, 4th ed. St. Louis: Elsevier, 2017, pp 407-410.
28 Hall-Fonte DL, Center SA, McDonough SP, et al. Hepatocutaneous syndrome in Shih Tzus: 31 cases (1996-2014). J Am Vet Med Assoc 2016;248:802-813.
29 Bach JF, Glasser SA. A case of necrolytic migratory erythema managed for 24 months with intravenous amino acid and lipid infusions. Can Vet J 2013;54:873-875.
30 Hnilica KA, Patterson AP. Symmetrical lupoid onychodystrophy. Small Animal Dermatology: A Color Atlas and Therapeutic Guide, 4th ed. St. Louis: Elsevier, 2017, pp 444-447.
31 Waisglass S. Claw disease in the dog: does your patient have symmetrical lupoid onychodystrophy (SLO)? Can Vet J 2018;59:796-798.
32 Freeman LM, Chandler ML, Hamper BA, Weeth LP. Current knowledge about the risks and benefits of raw meat-based diets for dogs and cats. J Am Vet Med Assoc 2013;243:1549-1558.
33 Sousa C, Stannard AA, Ihrke PJ, et al. Dermatosis associated with feeding generic dog food: 13 cases (1981-1982). J Am Vet Med Assoc 1988;192:676-680.



